16 January 2018
•3 minute read
Hemorrhoids (Piles) What Do You Do About Them?
What are hemorrhoids
Hemorrhoids are abnormal swelling of blood vessels lining the lowest part of the rectum and anus.
They developed when the veins in the anal canal get swollen and congested, just like the varicose veins in the leg, due to the weakness of the vessel wall and increased localized pressure in the vessels. With increasing age, the connective tissue degeneration leads to prolapsed blood vessels in the anus.
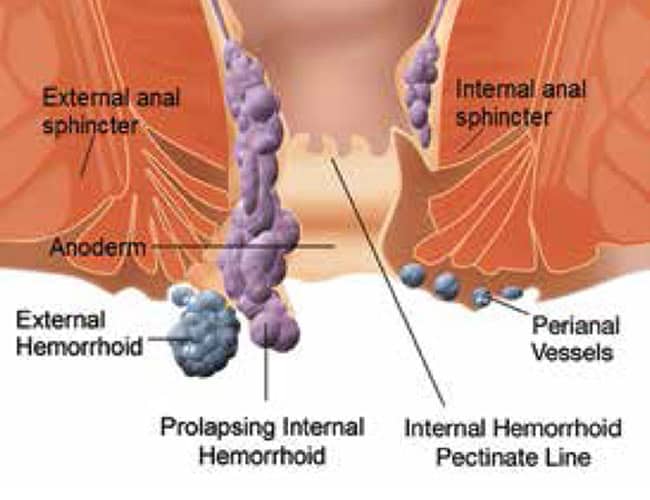
There are two types of hemorrhoids
- External hemorrhoids – which develop around the anus and the most uncomfortable ones. If blood clots are formed inside an external hemorrhoid, patients will have excruciating pain.
- Internal hemorrhoids – Can be found at the lower rectum. Usually painless.
Who will get hemorrhoids?
- Men – 60% of hospitalized hemorrhoid are male patients.
- Women – Usually will get them during pregnancy and after childbirth. The enlarging womb of the pregnant mother presses on the veins and causes blood to pool and vessels engorgement.
- Age – The risk increases with older people due to degenerative disease.
- Constipation – Frequent straining, decreased intake of fibre and fluid, prolonged sitting on the toilet all contribute to poor blood flow at the anal vessels.
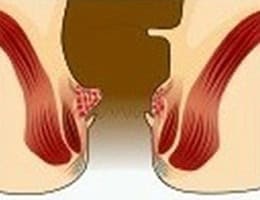
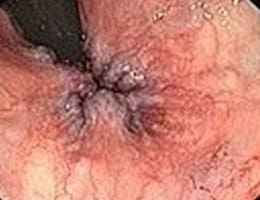
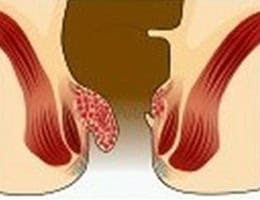
Internal hemorrhoid grades
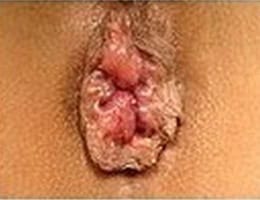
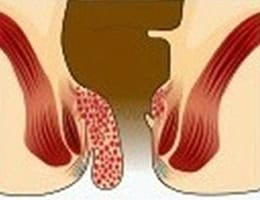
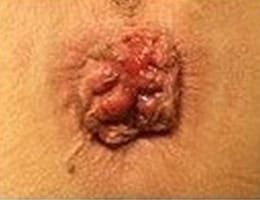
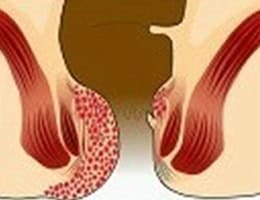
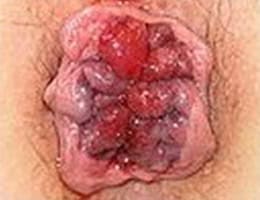
How are hemorrhoids diagnosed?
Patients will get bleeding during defecation, lump at the anus, pain, or even itchiness.
Your doctor might perform examinations and tests to confirm the diagnosis, such as proctoscopy (a device to visualize the anal canal) and colonoscopy (endoscopy of the large bowel and rectum, to rule out other causes of bleeding such as cancer or polyps.
What are the treatment option?
1. Diet and Lifestyle Modification
- Add more fiber intake in your food, and drink plenty of water to avoid constipation and straining. They soften stool and make it easier to pass, hence reducing pressure on hemorrhoids.
- Develop a regular bowel habit by exercising more, which will stimulate bowel movement. Make it a habit to go to the toilet at a scheduled time, and to sit on a toilet for a few minutes to encourage defecation.
- A sitz bath is a warm water bath with salt added in, to relieve itching, swelling and muscle spasm. Apply after each bowel movement for around 20-30 minutes for symptoms relief.
2. Medical Therapy
- Hemorrhoidal medications, topical cream and stool softener will help to shrink and decrease swelling at the anus and stop bleeding as well. They can be prescribed by your family doctors.
3. Daycare Procedures
- A number of minimally invasive procedures are available widely in the hospital, and patients do not need to be hospitalized to get treatment.
- Examples are rubber banding ligation, sclerotherapy, cryotherapy and infrared coagulation of hemorrhoids.
4. Hemorrhoidal Surgery
- Some hemorrhoids just can’t be managed by conservative treatment alone especially the bigger ones. Eventually, surgical treatment is the best option to treat the ‘stubborn’ hemorrhoids.
- Open Hemorrhoidectomy: If the large protruding hemorrhoid is causing pain and bleeding, this is the best option available. It has a 95% cure rate and less complication but also has a notorious reputation for being painful.
- Stapled Hemorrhoidopexy: This procedure treats prolapsed hemorrhoid and is less painful compared to a conventional hemorrhoidectomy.
- Other less painful procedures available are Laser Hemorrhoidoplasty and HAL- RAR (Hemorrhoidal Artery Ligation – Recto Anal Repair), but the success rate is much lower compared to surgical excision.
Hemorrhoids (Piles) What Do You Do About Them? – InfoMed Malaysia, Issue 24, Jan – Mar 2018
Share:
Was this article helpful?
16 January 2018
•3 minute read
Hemorrhoids (Piles) What Do You Do About Them?
Learn more about General Surgery in Columbia Asia
Learn MoreShare:
Was this article helpful?
Health Packages
Elevate your health with tailored health packages at Columbia Asia Hospital. Take charge of your health journey today.
12.12 CheckJer Health Package
RM140
Find Out MorePink October 2024
From
RM80
AIA Policyholders Self-pay Benefits
Pink October 2025
From
RM80
HLA Policyholders Promo: Influenza Vaccination
RM65
Find Out More
