15 February 2017
•2 minute read
Points To Consider When Diagnosing ‘Red Eyes’ in Primary Care Setting
Article credit : InfoMed Malaysia, Issue 20, Jan – Mar 2017
Patients regularly present to the general practitioners with complaints of red eyes. Although most of them suffer from the common viral conjunctivitis, it is important to bear in mind that there are other possible causes for red eyes that would require different modes of treatment and sometimes a referral to the eye surgeon.
Listed below are pertinent case mix that may aid in the diagnosis and management when a patient presents with red eyes.
Viral conjunctivitis
Redness, tearing, discharge and itchiness, usually starting from one eye and spreading to the other.
- History of contact with family members or colleagues with red eyes.
- Treatment is usually supportive with a cold compress, artificial tear drops, antibiotic eyedrops and oral anti-histamines.
- Referral to an ophthalmologist is necessary if the symptoms do not resolve after 5 to 7 days, if corneal involvement, or periorbital swelling due to pseudomembranes under the eyelids.
Allergic conjunctivitis
- The recurrent problem usually associated with allergic rhinitis and/or eczema, asthma.
- Usually, symptoms are worse in the mornings with the main complaints being bilateral itchiness and tearing.
- May have a discharge which is classically ‘stringy’ in nature.
- History coincides with exposure to allergens, most commonly dusty environment.
- Treated with ocular lubricants and topical anti-histamine/mastcell stabilisers.
- Referral required if symptoms persist, blurring of vision, eye pain or presence of any corneal opacity.
Episcleritis
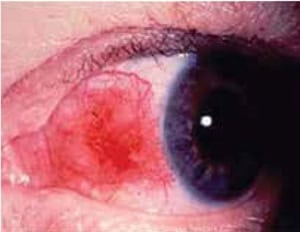
Figure 1 – Episcleritis
- Localised area of inflammation involving the superficial coats of the sclera of usually one eye.
- May sometimes present with a nodular lesion in the hyperemic region.
- May present with little or no discomfort with minimal tearing.
- Can be treated with a short course of oral non-steroidal anti-inflammatory drugs with topical lubricants.
- Will need a referral if symptoms persist more than five days, blurring of vision, significant pain or recurrent episodes.
Subconjunctival haemorrhage (Figure 2)
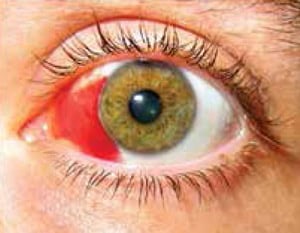
Figure 2 – Subconjunctival Haemorrhage
- It occurs due to bleeding in the area between the conjunctiva and the sclera due to rupture of the small, fragile conjunctival vessels.
- Usually spontaneous but may also be associated with history of forceful coughing/sneezing/ vomiting, straining, eye rubbing, uncontrolled blood pressure, trauma to the eye or base of skull fracture.
- Usually self-limiting and will resolve within two weeks by changing colour from bright to dull red, orange, brown, yellow then complete resolution.
Uveitis
- Refers to inflammation of the uveal tissue which is the middle coat of the eye.
- Maybe unilateral or bilateral.
- Associated with the blurring ofvision, discomfort, photophobia, tearing, floaters and redness of the eye which is usually more prominent around the cornea (circumciliary injection).
- Will need a referral to an ophthalmologist.
Acute angle closure
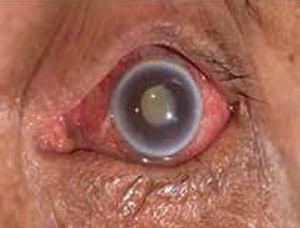
Figure 3 – Acute Angle Closure
- Usually sudden onset of unilateral pain, tearing, redness, photophobia, blurring of vision associated with headaches, nausea and vomiting.
- Hyperemic eyes, haziness of cornea with fixed or poorly reactive pupils with the eyeball feeling firm/hard to touch (always compare with the other eye).
- Needs urgent eye referral.
Red flags associated with red eyes that requires urgent eye referral
- History of contact lens usage.
- Trauma/foreign bodies especially of high-velocity in nature.
- Chemical injuries.
- Sudden loss or impairment of vision and severe eye pain.
Points To Consider When Diagnosing ‘Red Eyes’ in Primary Care Setting – InfoMed Malaysia, Issue 20, Jan – Mar 2017.
Share:
Was this article helpful?
15 February 2017
•2 minute read
Points To Consider When Diagnosing ‘Red Eyes’ in Primary Care Setting
Articles and Video
Learn more about Ophthalmology in Columbia Asia
Learn MoreShare:
Was this article helpful?
Health Packages
Elevate your health with tailored health packages at Columbia Asia Hospital. Take charge of your health journey today.
Pink October 2024
From
RM80
Columbia Asia 30th Anniversary Promotion “Maternity & Baby”
Pink October 2025
From
RM80
HLA Policyholders Promo: Influenza Vaccination
RM65
Find Out MoreAIA Policyholders Self-pay Benefits
12.12 CheckJer Health Package
RM140
Find Out More
