Hernia repair operations are commonly performed by the conventional “open” method in Malaysia. Some are performed laparoscopically. Laparoscopic hernia repair is a relatively new surgical technique to fix tears in the abdominal wall (muscle) using small incisions, a patch (mesh), and special cameras to view inside the body.
It frequently offers a more rapid recovery for the patient, less post-operative pain, and a quicker return to work and normal activities.
What is a Hernia?
A hernia occurs when the inside layers of the abdominal muscle have weakened, resulting in a bulge or tear. In the same way that an inner tube pushes through a damaged tire, the inner lining of the abdomen pushes through the weakened area of the abdominal wall to form a small balloon-like sac. This can allow a loop of intestine or abdominal tissue to push into the sac. The hernia can cause severe pain and other potentially serious problems that could require emergency surgery. Both men and women can get a hernia. You may be born with a hernia (congenital) or develop one over time. A hernia does not get better over time, nor will it go away by itself.
What causes a Hernia?
The wall of the abdomen has natural areas of potential weakness. Hernias can develop at these or other areas due to heavy strain on the abdominal wall, ageing, injury, an old incision or a weakness present from birth. Anyone can develop a hernia at any age. Most hernias in children are congenital. In adults, a natural weakness or strain from heavy lifting, persistent coughing, and difficulty with bowel movements or urination can cause the abdominal wall to weaken or separate.
Laparoscopic Hernia Repair is a technique to fix tears in the abdominal wall (muscle) using small incisions, telescopes and a patch (mesh). If may offer a quicker return to work and normal activities with a decreased pain for some patients. The scars are cosmetic and it allows inspection and repair of concomitant obturator, femoral and bilateral inguinal hernias in the same sitting.
Are you a candidate for laparoscopic Hernia repair?
Only after a thorough examination can your surgeon determine whether laparoscopic hernia repair is right for you. The procedure may not be best for some patients who have had previous abdominal surgery or underlying medical conditions.
What preparation is required?
- Most laparoscopic hernia operations require a short hospital stay, and therefore you will probably go home on the next day after the operation is performed.
- Preoperative preparation includes blood work, medical evaluation, chest x-ray and an ECG depending on your age and medical condition.
- After your surgeon reviews with you the potential risks and benefits of the operation, you will need to provide written consent for surgery.
- It is recommended that you shower the night before or morning of the operation.
- After midnight the night before the operation, you should not eat or drink anything except medications that your surgeon has told you are permissible to take with a sip of water the morning of surgery.
- Drugs such as aspirin, blood thinners, anti-inflammatory medications (arthritis medications) will need to be stopped temporarily for several days to a week prior to surgery.
- Quit smoking and arrange for any help you may need at home.
How is the procedure performed?
A laparoscope (a tiny telescope) connected to a special camera is inserted through a trocar, a small hollow tube, allowing the surgeon to view the hernia and surrounding tissue on a video screen.
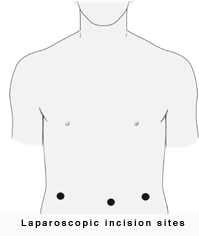
Other trocars are inserted which allow your surgeon to work “inside.” Three 1/2 to 1 cm incisions are usually necessary. The hernia is repaired from behind the abdominal wall. A small piece of surgical mesh is placed over the hernia defect and held in place with small surgical staples or sutures. This operation is usually performed under general anesthesia.
What happens if the operation cannot be performed or completed by the laparoscopic method?
In a small number of patients the laparoscopic method cannot be performed. Factors that may increase the possibility of choosing or converting to the “open” procedure may include obesity, a history of prior abdominal surgery causing dense scar tissue, inability to visualize organs or bleeding problems during the operation.
The decision to perform the open procedure is a judgment decision made by your surgeon either before or during the actual operation. When the surgeon feels that it is safest to convert the laparoscopic procedure to an open one, this is not a complication, but rather sound surgical judgment. The decision to convert to an open procedure is strictly based on patient safety.
What complications can occur?
Any operation may be associated with complications. The primary complications of any operation are bleeding and infection, which are uncommon with laparoscopic hernia repair.
There is a slight risk of injury to the urinary bladder, the intestines, blood vessels, nerves or the sperm tube going to the testicle.
Difficulty urinating after surgery is not unusual and may require a temporary tube into the urinary bladder.
Any time a hernia is repaired it can come back. This long-term recurrence rate is not yet known. Your surgeon will help you decide if the risks of laparoscopic hernia repair are less than the risks of leaving the condition untreated.
What should I expect after surgery?
Following the operation, you will be transferred to the recovery room where you will be monitored for 1-2 hours until you are fully awake.
Once you are awake and able to walk, you will be sent home.
With any hernia operation, you can expect some soreness mostly during the first 24 to 48 hours.
You are encouraged to be up and about the day after surgery.
With laparoscopic hernia repair, you will probably be able to get back to your normal activities within a short amount of time. These activities include showering, driving, walking up stairs, lifting, working and engaging in sexual intercourse.
Call and schedule a follow-up appointment within 2 weeks after you operation.
When to call your doctor
Be sure to call your physician or surgeon if you develop any of the following:
- Persistent fever over 39 C
- Bleeding
- Increasing abdominal or groin swelling
- Pain that is not relieved by analgesic drugs
- Persistent nausea or vomiting
- Inability to urinate
- Chills
- Persistent cough or shortness of breath
- Purulent drainage (pus) from any incision
- Redness surrounding your incisions that is worsening or getting bigger
- You are unable to eat or drink liquids
This information is not intended to take the place of your discussion with your surgeon about the need for laparoscopic inguinal hernia surgery. If you have questions about your need for hernia surgery, your alternatives, billing or insurance coverage, or your surgeons training and experience, do not hesitate to ask your surgeon or his/her office staff about it. If you have questions about the operation or subsequent follow-up, please discuss them with your surgeon before or after the operation.
THE ABOVE INFORMATION HAS BEEN TAKEN FROM THE SAGES WEBSITE FOR PATIENT INFORMATION
Share:
Was this article helpful?
Share:
Was this article helpful?
Health Packages
Elevate your health with tailored health packages at Columbia Asia Hospital. Take charge of your health journey today.
HLA Policyholders Promo: Influenza Vaccination
RM65
Find Out More12.12 CheckJer Health Package
RM140
Find Out MorePink October 2025
From
RM80
Pink October 2024
From
RM80

